Getting Started

The Benefits of At-Home INR Testing
At ACS, we pride ourselves on delivering safe, effective care in a few easy steps – which is why we have provided patients on warfarin with a reliable at-home INR testing service for over a decade. Here are a few of the ways the experts at ACS provide modern, exceptional care from the comfort of your home.
- Enrollment: ACS will assist you with all your enrollment needs, including connecting with your medical provider who will be the one to order the at-home INR testing and your insurance company for coverage verification.
- Training: Our talented team of training specialists will coordinate a personalized training session with you and teach you how to self-test and record your results.
- Procurement: We deliver all the state-of-the-art medical supplies you need to successfully self-test from home, including your digital PT/INT meter and testing strips.
- Support: We are here for you and our staff will stay connected with your medical provider to ensure you enjoy the best patient experience.
Patient Support

Frequently Asked Questions
Have questions about at-home INR testing? Our Frequently Asked Questions section covers many of the most common questions fielded by our customer support team.
ACS® Blog
Check out our latest articles about Advanced Cardio Services, INR testing, and more.mdINR® App

mdINR® App
With the mdINR® app, you get access to industry-leading anticoagulation management software that can quickly and efficiently keep you connected to your medical provider. Just submit your PT/INR self-test results directly through the application. After that, your medical provider can quickly review your results and provide you with the feedback you need. Download the mdINR app today!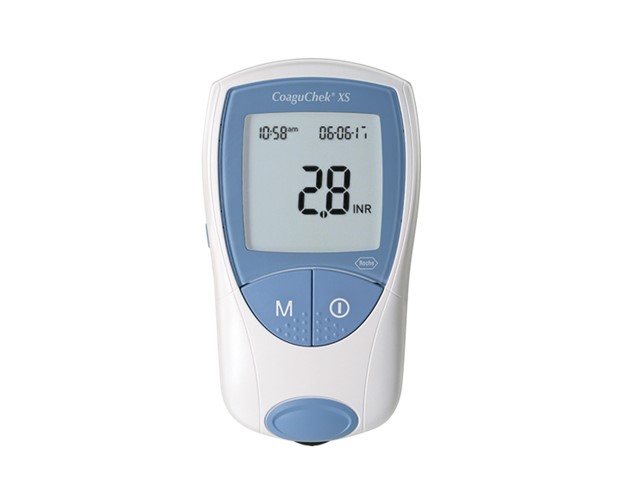
Choose ACS® Today
ACS is committed to assisting individuals on long-term warfarin therapy with a comprehensive anticoagulation program that allows patients to self-test for INR from the comfort of home. ACS provides industry-leading products, dependable services, and ongoing support that helps patients every step of the way.
If you are interested in learning more about how you can self-test for INR from the comfort and safety of home, contact us today.